Health & Sexuality Info
The Our Bodies Ourselves website features accurate information, compelling personal stories, and incisive feminist analysis on the health and sexuality of women and gender-expansive people.

Abortion
The majority of unplanned pregnancies end in abortion. These resources help us understand the medical procedure itself, as well as the policies that try to limit our right to choose whether we continue a pregnancy.

Breast Cancer
A new subject area on breast cancer is coming soon to Our Bodies Ourselves! The resources will be based on the work of Breast Cancer Action (BCA), who sadly closed after 34 years of addressing breast cancer as a public health and social justice concern. Our Bodies Ourselves is in the process reviewing and updating their materials.
Contraception
There are many forms of birth control. Detailed, accurate information about contraceptives helps us find the best options for ourselves, and helps us support each other's reproductive rights as well.
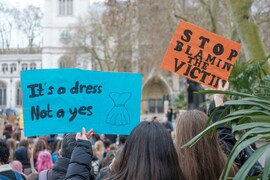
Gender-based Violence
The resources in this section look at the kinds of violence we experience, our struggle to survive and heal, and the movement to end gender-based violence.

Growing Older
How can we navigate aging – and confront ageism – as women and gender-expansive people? These materials help us to understand our changing bodies and circumstances, and to celebrate our diverse identities as we grow older.

Heart Health
The heart is strong, flexible, adaptive, and central to our well being. Gender and biological sex are often overlooked factors in our cardiovascular conditions, including diagnosis and treatment.
Menstrual Cycle
Our menstrual cycles raise many questions, from how to take care of our menstrual health to removing the stigma around periods and hygiene products.

Menopause & Perimenopause
The end of our menstrual cycle may come with varying symptoms, at different ages. Research and personal stories alike help us grapple with the often misunderstood biological and social processes of perimenopause and menopause.

Mental Health
The resources in this section offer critical insight, empathetic support, and vital perspectives on mental health. The readings, videos, and stories center women and gender-expansive people, and encourage us to challenge the status quo.

Pregnancy & Birth
Pregnancy, giving birth, and parenting a newborn are major (and often daunting) experiences in our lives. This section’s trustworthy information and first-person accounts help us to understand and prepare for those experiences more confidently, within a framework of birth justice for all.
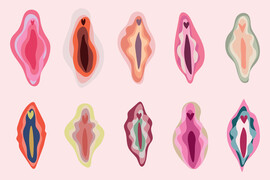
Sexual Anatomies & Sexual Health
These resources help us understand the way our sexual and reproductive systems work, how they interact with other body functions, and how they are connected to our environments, our daily lives, and our overall well-being.
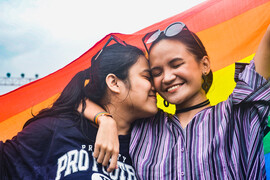
Sexualities, Gender, and Relationships
Sexuality can be a source of deep pleasure and of great pain. This section looks at the full spectrum of gender identities, sexual identities, and intimate relationships.

