Breast Cancer Study Encourages Reconsideration of DCIS (Ductal Carcinoma In Situ) and its Treatment
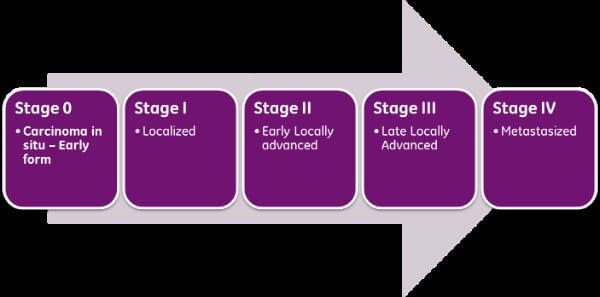 Stages of breast cancer, beginning with ductal carcinoma in situ
Stages of breast cancer, beginning with ductal carcinoma in situ
By Mary E. Costanza, MD — August 31, 2015
Women who are diagnosed with a very early stage of breast cancer usually undergo some type of surgery with the hope that it will eliminate their risk of developing invasive breast cancer. The most common treatment is lumpectomy followed by radiation, though some women opt for a mastectomy or even a double mastectomy, which involves removing a healthy breast as well.
A new study published this month shows that in most cases, treatment does not affect a woman’s outcome, throwing into question whether surgical treatments have been overly aggressive and overused.
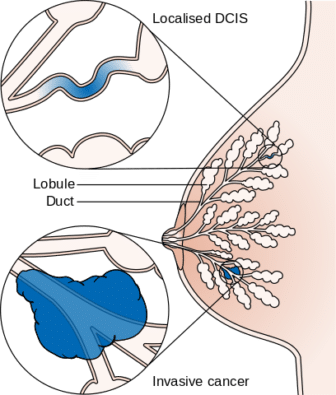
This early cancer stage is known as ductal carcinoma in situ (DCIS) and is commonly referred to as Stage 0. With DCIS, abnormal cells develop from cells that line the milk ducts; however, these abnormal cells have not invaded the surrounding breast tissue.
Increased mammogram screening has led to an increase in DCIS diagnoses in recent years. The American Cancer Society estimates that about 60,290 new cases of DCIS will be diagnosed in women in 2015, along with nearly 232,000 new cases of invasive breast cancer. About 40,290 women will die from breast cancer this year.
In August, the cancer journal JAMA Oncology published two important papers about DCIS that tests our understanding of DCIS and its role in invasive breast cancer. The first, “Breast Cancer Mortality After a Diagnosis of Ductal Carcinoma In Situ,” found that half the time invasive breast cancer develops, it has not developed from a prior DCIS. This finding challenges the orthodox view that DCIS is the original tissue from which most invasive ductal carcinomas (the most common form of breast cancer) develop.
This probably means DCIS is a marker – a woman may have cells somewhere in the breast that either are or will become invasive cancer, but these cells are currently undetectable. In other words, DCIS is functioning more as a risk factor rather than a direct cause in at least half of all breast cancer deaths.
According to the study:
• 1.1 percent of women with DCIS had died of invasive breast cancer by the 10-year mark and 3.3 percent of women by the 20-year mark. These rates, while low, are almost twice that for the U.S. population.
• More than half the breast cancer deaths in DCIS women were not associated with an invasive in-breast recurrence. This fact suggests that local therapy alone is not enough to treat “aggressive” DCIS.
• Local therapy (surgery and/or radiation therapy) decreased the in-breast invasive cancer rate. However, it did not reduce the death rate from invasive cancer. DCIS that did recur in the breast as invasive disease was associated with a higher mortality rate.
This study is important because it is huge – reporting on over 100,000 women with DCIS – and because it is based on well-established survey data from 18 different U.S. cancer registries. Its findings are similar to those from a much smaller and earlier study from Sweden. The fact that two different studies have reported the same general conclusions makes these findings more believable.
A number of factors were identified that predict whether invasive breast cancer and death are more likely to occur. The death rate was higher in black women and in women who were diagnosed before age 35, making both of these key risk factors. Additional risk factors include:
• a DCIS that is larger than 1 cm. (1/2 inch).
• a DCIS that is insensitive to hormones (no estrogen or progesterone receptors).
• a DCIS that is of higher grade (more cancer-like).
• a DCIS showing increased cell death (comedonecrosis).
While these factors have been suspect for some time, having them confirmed in such a large study makes us more comfortable in sorting out which DCIS patients are more or less likely to die from an invasive breast cancer.
For DCIS types associated with high risk factors, it may be more beneficial to consider systemic therapies, like chemotherapy or hormonal therapy.
The second paper published in JAMA, “Rethinking the Standard for Ductal Carcinoma in Situ Treatment,” reviews treatment options in light of these new findings.
So, what should you do if you are diagnosed with DCIS?
As always, the best advice is to get a second opinion, and the best place to get it is at a well-known and respected breast cancer center. Their experts will evaluate your risks and discuss with you all the treatment options available. With the identification of factors more likely to be associated with death, there is now the real possibility of tailoring treatment depending on a woman’s individual risk.
Remember the good news is that all DCIS tumors are not the same – some are associated with higher risk for breast cancer death; others are not.
In addition, 97 percent of the time, DCIS does not result in a death from breast cancer. And if you have few or none of the high-risk conditions, your prognosis is even better that 97 percent.
Mary E. Costanza, MD, is a professor of medicine at University of Massachusetts Medical School.

Thanks for this great article and insights. I was diagnosed with DCIS in 2001 and opted for a mastectomy & reconstruction and am now thriving.
Writing has always helped me survive. For this journey, my book, Healing With Words: A Writer’s Cancer Journey, has helped me and others in a big way and I hope my teaching others to write to heal will help others.
Peace,
Diana
Comment
The low but consistent incidence rate of invasive breast cancer deriving from ductal in situ carcinoma (DCIS) justifies that the usual surgical and adjuvant therapy of high grade DCIS is not always capable of ensuring a tumor-free life, while low grade DCIS is perhaps superfluously over treated.
Appropriate estrogen receptor (ER)-signaling is the chief safeguard of genomic stability in strong interplay with DNA-controlling and repairing systems, such as BRCA-genes and their protein products [http://goo.gl/EsB1bK]. Detection of DCIS by mammographic screening may be regarded as an early marker of disturbed hormonal, metabolic and DNA-stabilizer equilibrium, since the female breast is exquisitely sensitive to the defects of estrogen signaling [http://goo.gl/xRh4wL]. The stronger the defect of cellular estrogen surveillance, the higher is the probability of DCIS development with high-risk characteristics.
Among young cases with active ovarian estrogen synthesis, the relatively higher risk of poorly differentiated DCIS may be attributed to the low incidence rate of more successfully suppressed ER-positive cancers rather than an excessive inclination to ER-negative tumors. Moreover, among dark-skinned American women, the higher risk of developing poorly differentiated DCIS and the higher breast cancer mortality rate as compared with white women are associated with estrogen deficiency and further hormonal defects. These endocrine disturbances may be explained by the incongruence between their excessive pigmentation and the poor light and sunshine exposure of North-America.
[http://dx.doi.org/10.2174/157489212801820048].
In women, during aging, progressive weakening of estrogen signaling and the associated gene stabilizer mechanisms are dangerous systemic processes [http://goo.gl/yiYszF], despite any usual, aggressive treatment of DCIS. In patients having increased risk of invasive breast cancer, natural estrogen substitution is the optimal risk-reducing therapy aiming the stabilization of gene regulatory processes and the apoptotic death of accidentally initiated tumor cells [http://dx.doi.org/10.2147/dddt.s89536]. By contrast, antiestrogen treatment against tumor recurrence may be risky, being effective only in such genetically proficient women who are capable of strong, counteractive upregulation of estrogen signaling. Tumor growth may be provoked by de novo or acquired antiestrogen resistance being associated with the missing capacity of patients for the extreme upregulation of estrogen signaling or with the exhaustion of defensive counteractions by excessive antiestrogen administration [http://dx.doi.org/10.2147/dddt.s89536].
In conclusion, in cases of DCIS which have been diagnosed, the most important preventive strategy against invasive breast cancer development is to combine lumpectomy with strict control and maintenance of estrogen signaling over a whole lifetime.
Zsuzsanna Suba
Clarification: DCIS is *not* cancer. It is termed “pre-cancer” which means one may or may NOT develop breast cancer with these cells. Calling it cancer is a huge part of the problem and why way too many women are unnecessarily having their breasts cut off because doctor’s tell them to. Like you said, it’s a risk factor. As Dr Esserman, head of the UCSF Breast Center said, “Ductal carcinoma in situ is not cancer, so why are we calling it cancer?” (source: NY Times, http://well.blogs.nytimes.com/2013/07/29/report-suggests-sweeping-changes-to-cancer-detection-and-treatment/?_r=0). I’m so frustrated by these “hero” stories of people “battling breast cancer” who actually did NOT have cancer but were told they did by the deceptive term DCIS, and then were told surgery and chemo were the only things to ‘save their lives’ when, like you said, 97% of people with DCIS don’t die from breast cancer.
Aimee, it’s strange to me that someone would say that DCIS is not cancer. IT IS CANCER – IT JUST HASN’T SPREAD. I was diagnosed with DCIS High Nuclear Grade Level III with Comedo-Necrosis. I have had two lumpectomies and so far, have not been able to get clear margins. I am scheduled for a third lumpectomy and if that doesn’t come back clear, I’ll have a mastectomy followed by radiation and possibly chemo. So to hear you say that I do not have cancer is insulting and minimizes what I am going through. Either you are ignorant or a pompous ass. Please know what you are talking about before insulting people who are going through this issue.
I am wondering how your 3rd excision went. I am in the same boat at the present time. Thanks for your reply.
I have breast cancer and i have been treating it for the past 2 years. I want for different check ups, therapy sessions and took prescribed drugs but it didnt cure it. Until i contacted a physician through the internet, and explained my situation to him. He sent me cannabis oil (marijuana) and after a few months the lump in my breasts vanished and dissolve completely . You can reach him via email on davidcancertreatment@gmail.com
Good to know. I have been diagnosed with intermediate and high grade dcis in the right breast with necrosis and calcium, B5A
Prominent periductal inflammation.Convincing evidence of invasive cancer is not evident.
What is your advice about that ?
Should I be treated and how ? Surgery, or something different?
I look forward to your reply,
Best Wishes,
Alma De Pietri
[…] http://www.www.ourbodiesourselves.org/2015/08/breast-cancer-study-encourages-reconsideration-of-dcis-duc… […]
[…] Image source. Describing breast cancer. […]
please show me graphic of breast cancer stage 1
[…] Breast Cancer Study Encourages Reconsideration of DCIS (Ductal … […]